Pelvic Disease

Pelvic inflammatory disease is an infection of the uterus, endometrium, fallopian tubes and ovaries that may be characterized as acute, subacute, recurrent or chronic.
Most infections are caused by bacteria such as chlamydia or gonococcus, but viruses, fungi and parasites can also lead to an inflammatory process. Infectious diseases of the pelvis can develop as a result of unprotected sexual intercourse, intrauterine manipulation, vaginal infections, poor feminine hygiene, or misuse of feminine hygiene products. Rarely, the cause may be a complication after labor or pelvic surgery.
Symptoms:
- Pain in the abdomen and pelvic area, accompanied by vaginal discharge. The intensity of pain varies from mild to significant, interfering with daily routine of women''s lives. Pain worsens during sexual intercourse;
- Fever, sometimes accompanied by fatigue and headache;
- Sensitivity to palpation of the lower abdomen;
- Increased number of leukocytes in a general blood analysis;
- Uterine bleeding, not related to the monthly cycle;
- Nausea and vomiting.
Treatment of pelvic inflammatory disease typically requires the use of antibiotic therapy. The choice of drugs is made by the attending physician, taking into account the patient’s history, checkup and additional methods of examination. Medicine is normally taken in a tablet form, but may also be given by an intramuscular injection. Sometimes the anti-inflammatory treatment is carried out using steroids. In the most severe cases, drugs may be administered intravenously in the hospital. If necessary, the doctor will prescribe pain medication. Surgery is required in case of any complications caused by the inflammation. The importance of drug treatment is extremely high.
Ectopic pregnancy: "Ectopic pregnancy" denotes a complication of pregnancy, during which the embryo begins to develop outside of the uterus, in another organ of the female reproductive system. Typically, ectopic pregnancies develop in the fallopian tubes. In rare cases, it occurs in the ovary, the abdomen or cervix. An ectopic pregnancy occurs once in 100 births.
There are several conditions that can result in an ectopic pregnancy:
- a structural disorder of the fallopian tubes caused by previous inflammation;
- processes in the pelvic organs;
- surgeries in the abdominal area;
- endometriosis;
- malformations of the fallopian tubes;
- unidentified reasons;
- a pregnancy resulting from infertility treatment.
If an ectopic pregnancy is not diagnosed promptly and cured properly, a woman may suffer from a serious health damage, including danger to her life.
Treatments for ectopic pregnancy range from medication to conservative therapies and surgery. The choice of treatment is made by the attending physician, who often requests a medical consultation from another specialist. Most women with an ectopic pregnancy undergo laparoscopic surgery, in which the surgeon uses miniaturized equipment that does not require an incision in the abdomen. A laparoscopic operation is performed under general anesthesia, and is a faster and easier procedure than open surgery. Many ectopic pregnancies terminate on their own, in a process similar to spontaneous abortion. In these cases, the woman does not require additional medical intervention except for a compulsory examination in hospital to determine that the pregnancy is fully terminated.
Micro-invasive surgery - Endoscopy
In the last decade, there have been revolutionary changes in surgery, including gynecological surgery, related to the advent of endoscopic therapies and surgical interventions. Endoscopic surgery is a minimally invasive surgery that does not require abdominal incisions, in which lies its uniqueness. Endoscopic surgery is big surgery through a small incision.
To monitor the internal organs during an endoscopic procedure, physicians use light from optical fibers, coupled with a miniature video camera that is inserted into the body through a small opening in the abdominal wall. The surgeon can then perform the operation inside the body while observing it on a special screen.
When the optical fiber is inserted through a hole in the abdominal wall, usually through the navel, such a procedure is termed laparoscopic (from the word "laparo" - the abdomen and “scop” - watch) surgery. If the optical fiber is inserted through the vagina and cervix into the uterine cavity, it called hysteroscopic surgery.
The emergence of microinvasive surgery has significantly improved surgical treatments. It dramatically reduces the period of hospitalization, the intensity and duration of postoperative pain, accelerates healing and, since scarring is greatly reduced, improves cosmetic results. It is not surprising that both the surgeons and the patients express a growing need for surgeries using these advanced methods.
Due to endoscopic techniques, operations that used to require a long stay in a hospital bed and a considerable period of postoperative recovery may today be performed in hospital overnight. Even such complex operations as hysterectomies only take 24 hours when performed laparoscopically.
Laparoscopic approach
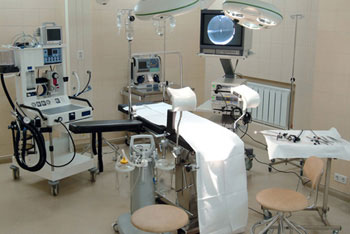
Laparoscopic surgery is the preferred method today in Chaim Sheba Hospital (Israel) for treating ovarian cysts, ectopic pregnancies, medical scrapings of the endometrium, and removal of the fallopian tubes, ovaries, or adhesions in the pelvic area.
Women, who have developed fibroids in the uterus, often suffer from heavy uterine bleeding. Traditionally, the main treatment for this problem was the removal of the uterus. For such cases, endoscopy offers a better alternative in the form of removing the fibroids while preserving the uterus, or cauterization of the endometrium by hysteroscopic approach.
Due to laparoscopy, fibroids or the uterus can be removed, and the patient enjoys all the benefits of this surgical approach. Laparoscopic procedures are used today in treating polycystic ovaries, endometriosis, adhesions and treatment of diseases of the fallopian tubes.
There is no doubt that the number of women, subject to large surgical incisions performed for treatment of the ovaries, uterus, and even the bladder (for example, in the case of urinary incontinence) will steadily decline, because laparoscopy facilitates a much more rapid recovery.
Hysteroscopic approach

Women, suffering from infertility, irregular or heavy uterine bleeding, and those, who are found to have a tumor, may undergo examination, including hysteroscopic inspection, without anesthesia.
To perform hysteroscopy, Sheba's doctors use the latest thin optical fiber inserted into the uterus to display and examine the uterine cavity. Depending upon the results of diagnostic hysteroscopy, they will determine the necessity of surgery.
Hysteroscopic surgery is used to treat women suffering from excessive or irregular uterine bleeding, removal of fibroids, polyps or cauterization of the uterine mucous membrane. Hysteroscopy is also used in the treatment of uterine congenital defects, for example, immature uterus in women with repeated miscarriages, and treatment of intrauterine adhesions (the mechanical cause of most female infertility).
Research
The doctors in the Gynecology Department regularly perform clinical and laboratory research to advance their knowledge and refine the methods to treat:
- massive uterine bleeding, to prevent removal of the uterus;
- infertility as a consequence of intrauterine adhesions;
- complications after hysteroscopic operations;
- heavy uterine bleeding or other bleeding disorders in women after pregnancy termination;
- miscarriage in early pregnancy and solutions such as an alternative cross-linking of the cervix.
In obstetrics, hysteroscopy is used in such treatments as suturing the cervix to cure cervical insufficiency (ischemic-cervical insufficiency), termination of pregnancy due to chromosomal defects, or medical abortion in early periods (up to 21 weeks).
Hysteroscopic treatment is also used to complete medicinal abortion, since it is performed to remove the placenta, which remains after the curettage or birth.




