Brachytherapy
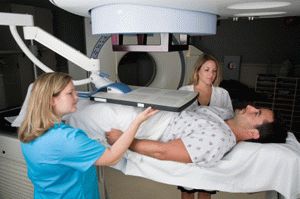
Brachytherapy is an innovative approach to cancer treatment that is widely used in modern radiotherapy. Its name comes from the Greek word meaning ‘a short distance’. The main feature of brachytherapy is the concept of locating radiation sources inside the body, as close to the cancer-affected organ as possible, or even inside of it. It is sometimes called internal radiation.
Brachytherapy is used to stop the growth and reduce the size of malignant tumors in organs such as the prostate gland. This approach is often used in conjunction with alternative cancer treatments, including chemotherapy, external beam radiotherapy and others.
The main difference from other types of radiation therapy is a precise location of the radiation source. Placing the radiation source directly into the affected area of the organ greatly increases the effectiveness of treatment, because the radioactive rays reach only a very restricted area near the source. This advantage is important in cases when the malignancy is unstable and changes its position. Brachytherapy permits precise location of the radiation source, and greatly reduces the possibility of complications and increases the chances for successful treatment.
Another benefit of brachytherapy is the significantly shorter duration of the irradiation treatment compared with external radiation therapy. In most cases, the number of brachytherapy procedures is minimal, and the time intervals between them are much shorter. This option of treatment is preferable, because large intervals between treatments significantly increase the risk of relapse. Moreover, since the treatments occur faster and on an outpatient basis, patients usually find it easier to tolerate this type of radiotherapy.
Brachytherapy is the main method used to treat prostate cancer. During the procedure, the radiation source (often in the form of microcapsules or grains) is placed inside the tumors of the affected organ. The microcapsule usually remains inside the prostate for several months until the radiation disappears completely. After the procedure, it cannot be removed from the patient, but it is not harmful to the patient's health.
An alternative to this kind of treatment is temporary brachytherapy. This technology is based on introducing radiation sources for a relatively short period of time. For example, the radiation source may be introduced into the patient two-three times within 48-72 hours. To enhance the effectiveness of radiotherapy, a combination of the above methods is often recommended.
However, the general understanding is that permanent brachytherapy is a more effective method of treatment for patients, whose cancers have been detected at an early stage. It is very important in this situation to consult an experienced and licensed specialist, who can take into account all of the factors that play a role in a successful procedure.
The first stage of the procedure includes determining the size of the prostate. This is carried out using ultrasound equipment. Next, the physician calculates the quantity and optimal placement of the radiation sources or seeds, which are titanium beads on special rigid fibers. Inside of each seed is iodine-125. At this stage it is important to achieve uniform distribution of radiation around the damaged organ. During the second stage of the procedure, the radioactive seeds are placed into the patient's prostate gland with special needles. The grains remain in the patient's body, creating the necessary radioactivity, which is generally not quenched for about 60 days. Since the grains are located inside the body, irradiation normally does not extend beyond the patient, and is not dangerous to others around him.
Currently, brachytherapy is used widely around the world and helps a vast number of patients diagnosed with prostate cancers. This approach is characterized by a high rate of success and low rate of complications. Compared with the highly effective method of removing the prostate (prostactomy), the risk of side effects, such as problems with urination, incomplete sexual function and so forth, is much lower by brachytherapy.
Cystoscopy
Cystoscopy is a widely used procedure used to examine the patient's bladder. It is carried out using a special optical device, called a cystoscope. The cystoscope consists of a long tube that is gradually introduced through the urethra into the patient's body until it reaches the bladder, which allows the physician to analyze the state of the urethra. Since this procedure is quite painful, especially for men because of the long urethra, a local anesthetic gel is frequently used to numb the area.
The cystoscope enables the physician to diagnose various diseases or pathologies of the urethra and bladder, to detect possible benign or malignant tumors in these organs, and to spot infections, possible defects of the organ, trauma, and foreign bodies. Cystoscopy is also frequently used for surgical interventions in various ailments of the genitourinary system.
Some kinds of surgeries, during which the device may be used, include operations on the bladder, prostate or urethra, treatment of ulcers and infections, removal of stones, biopsy, and lavage of the urethra, as well as treatments of other problems leading to enuresis. A cystoscope is a miniature device, so it is used mostly by minimally invasive procedures. Because this tool removes the need for abdominal surgery and the opening of the abdominal cavity, it reduces the likelihood of bleeding.
An important advantage of cystoscopy is that there is no need for hospitalization. This kind of surgical intervention usually requires the patient to remain in the hospital for a much shorter period of time than other procedures.
Unfortunately, cystoscopy cannot be recommended in all cases. Physical injuries and defects of the urethra, as well as some infections and inflammatory processes, require other methods of treatment. Also, if the patient has recently used anticoagulants, the use of this procedure may also be contraindicated. Before cystoscopy, the use of such drugs should be interrupted.
Hypospadias
Hypospadias is a congenital malformation of the genitourinary system observed in some men. In the case of hypospadias, the urethral opening is not located in the usual place - in the center of the glands of the penis, but a little away from the central zone. Sometimes there are cases when this opening can be covered wi
th the foreskin (completely or partially) or the urethral opening is not located directly on the penis, but in the nearby area of the perineum (behind or in front of the scrotum).Very often hypospadias are accompanied by other developmental defects of the genitourinary system, such as congenital curvature of the penis, external fusion of the reproductive system, narrowing in the urethra, abnormalities of the foreskin, both internal and external genitals, or other anomalies and physical defects.
It may seem that hypospadias is a rare developmental defect, but it actually occurs quite often—one or more per 200-300 male births, according to experts. Until recently, the exact factors that lead to such complicated defects, as hypospadias, have not been identified.
Specialists now suggest that these complications may result from abnormalities in the mother's body, influence of hormones, as well as negative external impact, during embryonic development. There may also be a hereditary predisposition to the disease, so genetics may also play a significant role.
Unfortunately, hypospadias is a serious disease, indicating a very serious problem that should be corrected. In particular, by newborn infants with such anomalies, it is sometimes not possible to determine their sex accurately. Some males may fall into a group known as "hypospadias without hypospadias”. In these cases, a shortened urethra leads to a distortion of the penis, rather than the urethral opening not being located at the proper place. In such a situation, a man is unable to enjoy a full sex life, because the shortened urethra cannot be stretched, and either causes painful erections, or makes them quite impossible.
Hypospadias sufferers quite often do not experience greater discomfort in normal life than other men. The most common issues are the inability to urinate normally, because the urethral opening is located in an unusual place.
Hypospadias can also be associated with impaired reproductive capacity, since an abnormal placement of the urethral opening may hinder the ejaculation and placing the sperm into a woman's body. In addition, there may be sexual difficulties due to unusual curvature of the penis. These defects of the male reproductive organs can lead to infertility or other problems.
These birth defects may also have a negative impact on the psychological state of a man. In order to avoid emotional problems and psychological disorders later, experts recommend starting treatment of this disease at an early age, literally from the first year of a baby’s life. In adolescent boys, structural features of the penis and urinating with hypospadias can result in an inadequate reaction of peers and cause serious psychological trauma to the child. Similar effects can occur in adulthood. In those cases, curvature of the penis in particular can cause impotence, which has both physical and psychological causes.
Currently, there are several types of operations to relieve hypospadias. After a consultation with a specialist, the patient will be offered the most appropriate type of surgery. Some of the factors taken into consideration include the degree and type of deformity, the location of the opening for the urethra, and whether it is necessary to extend and reconstruct the urethra. To reconstruct or elongate the urethra, the mucous membrane tissue from the bladder, appendix, circumcision or other areas of the body can be used.
In complex situations, surgical intervention may be carried out in several stages until the full restoration of the natural form and functions of the damaged organs or parts of the urogenital system is completed. Such operations can be conducted in a child in the first year and a half after the birth, but they are also suitable for patients of any age. Following the surgery, the patient is on bed rest with a urinary catheter for some period of time. In most cases, the rehabilitation process takes a maximum of 6-8 weeks. If any additional surgeries are needed, they are usually carried out after complete rehabilitation of the patient.




