Knee Arthroplasty (Replacement)
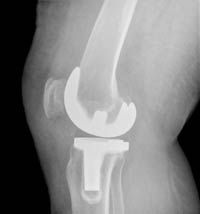
The procedure of arthroplasty or knee replacement is one of the most widely used and effective methods to restore function and mobility of the knee. The essence of this operation is to replace the injured or diseased knee joint with a new, artificial one.
In cases of serious injuries or degenerative changes in cartilage and other tissues of the knee joint, this method is sometimes the only alternative of full recovery of knee motor function. Knee arthroscopies were first performed in the 1970s, but nowadays the arthroplasty procedure is a routine operation widely used around the world.
Due to the vast experience gained by modern physicians and surgeons, joint replacement is a procedure of intermediate complexity, not associated with any high risk. Moreover, it has a very high percentage of successful outcomes.
The knee joint is, of course, a very complex and essential element of the musculoskeletal system. The joint connects the tibia and femur bones of the lower and upper leg, and it is covered by the patella. The knee joint regularly experiences tremendous pressure when we are walking, running or performing any other motion in a vertical position.
Various forms of osteoarthritis or osteoarthrosis of the knee joint may require arthroplasty. Under osteoarthritis we understand a series of degenerative diseases of different natures, when the pathological processes initially occur in the inner cartilage, gradually transforming then the entire joint - its ligaments, muscles, and adjacent parts of the bones and so on.
In more than two out of three cases with this disease, it is not possible to avoid severe joint injuries. Very often as a consequence of this disease, the patient experiences joint pain, loss of mobility and disability. With the help of X-rays, the doctor can diagnose this disease in 10-14% of patients between 45 and 50 years. The main symptoms are visual changes and deformation, as well as pain in the knee joint. In the early stages of the disease, pain usually occurs only under heavy mechanical loading and is of short duration, but in the later stages, pain in the knee joint is amplified even under a minimal load, persists even at rest, and brings much discomfort at night and in the morning hours.
Another large group of joint diseases includes arthritis. These illnesses are inflammatory, and frequently manifest in the form of rheumatoid arthritis and traumatic arthritis, which are hereditary and often occur in people older than 50 years. This type of disease, especially in the knee joint, can be caused by trauma, viral or other type of infection, ankylosing spondylitis or other diseases. If the function of the joint is seriously impaired, there is a lot of pain and discomfort, and the patient is unable to maintain their old lifestyle. Instead of conservative treatments for these symptoms, arthroplasty is assigned, if there are no clearly defined contra-indications. In such cases, it is also very important to consult and undergo a full examination by a qualified orthopaedist. After all, procedures such as joint replacement should take into account many factors, ranging from the pain intensity to the degree of restriction of physical activity. Knee arthroplasty operations can be successfully carried out in both older and young patients.
Prior to a surgical intervention, a series of tests, including X-rays and others, are performed in order to establish the degree of joint pathology and to select a suitable prosthesis. It is also imperative to fully examine the patient''s health status, so a series of tests should be performed, including blood test, urinalysis, etc. If a patient does not have a chronic disease, as a rule, the surgery is recommended.
Surgery
The arthroplasty procedure itself usually lasts about 2-3 hours. First, surgeons expose the joint capsule and remove part of the rear surface of the patella and the tissues surrounding the joint. It is crucial to keep intact all the ligamentous structures of the operated joint. Then, a new artificial strip in a shape ideally suited to the articular surfaces, is installed on the cleaned surface of the bone adjacent to the operated joint. At the final stage of the procedure, the surgeon installs a small drainage tube that will remove blood and other fluids from the wound.
Artificial prostheses installed during this procedure can be divided into three types:
- Prostheses with cement fixation
- Prostheses with cement-free fixation
- Combinations of the above two types
Generally, cement-free prostheses are used for younger patients, and cement and combined prostheses are for older patients. The possibility of combining prosthetic devices is achieved due to flexibility and interchangeability of the prosthetic parts and components, made from high quality materials like metals, ceramics and others. Nowadays, since there is high market competition of components and system implants, it is possible to use the most universal, high-quality and most appropriate prosthesis in each case.
Unfortunately, as in cases of other surgeries, this procedure also has the potential for undesirable side effects and complications. They can be divided into two groups: those related to the results of the procedure, and those associated with exacerbations of the patient''s existing illness. However, complications and unintended consequences can mostly be avoided successfully if pre-surgery tests were carried out properly; if after the procedure the patient receives prophylactic anticoagulant and anti-inflammatory therapy in the postoperative period; and if the patient closely follows all the instructions and advice of the doctor during recovery.
As a rule, during the first 24 hours after the arthroplasty procedure, the patient can shift around and find a more comfortable position in bed. The next day he/she can sit up, do breathing exercises, and carry out some remedial static exercises for leg muscles. On the third day, doctors usually allow the patient to rise to their feet and move cautiously. About 10-11 days after the procedure, the sutures are removed. Once the patient has been discharged, the doctor usually advises the patient to undergo a special rehabilitation program, specified for arthroplasty.
For all patients who have undergone arthroplasty, it is recommended to significantly reduce the load on the knee during the first 2-3 months after their surgery. At the same time, when moving is necessary, they should use a cane or other type of support. After 3-4 months, the patient can usually return to their previous activities. However, after knee replacement surgery, patients should completely abandon active sports, long walks, and especially weight lifting.
These recommendations are crucial to the health of the patient, but they are also necessary to prolong the life of the prosthesis. After all, even the most durable prostheses are subject to wear, and in the case of high loading on the joint, the prosthesis may fail earlier than usual, and cause a lot of inconvenience to the patient, including the need for a second arthroplasty. With the normal use, the prosthesis lasts up to 9-12 years in 85-90% of patients.
Increased loads usually lead to deterioration of the polymer linings, the loosening of prosthesis, and the deterioration of cements, with which the prosthesis is attached to the bone. In case of such deterioration, there is the need in another operation, known as "auditing". Thus, to use of prosthetic knee joints long and successfully, you should consider the following important factors, like adherence to the rules and guidelines for such a prosthesis; high-quality prosthetic arthroplasty procedures, and the skills of a top quality, experienced surgeon.




